The first time I saw fentanyl was on a spoon, in my hand, as I stood over my friend screeching for air on my bedroom floor.
Growing up together in Alberta, Tyson* and I experimented with the usual — hash, shrooms, weed — but he was always more enamoured with pharmaceuticals. The most innocent medicine bottles, some labelled with his mom’s name, didn’t just sharpen his focus, they washed away his social anxieties. In Toronto, where he moved for school, he lost himself in an array of prescription opioids — OxyContin, Dilaudid, Percocet, the whole gamut of “hillbilly heroins” and, when he was desperate, the non-hillbilly variety, too. Last year, shortly after shooting smack for the first time, he reached out to his family to pull him back West. Tyson thought he’d sober up with their support.
Everyone else was kept in the dark, though I suspected he was abusing something. What else would explain his frenetic phone calls, ever-changing numbers and jobs, petty lies and constant borrowing? But denial is practically an opioid in itself. I was just happy to see him again.
Within 20 minutes of his visit, I found Tyson leaning on my bathroom wall, clenching his smashed up phone, muttering to the light switch. When I tried to guide him onto a bed, his respiratory drive shut down and he collapsed like a faulty crane. My wife, who was studying for nursing school in another room, overheard the commotion and rushed to the bedroom.
She had me roll him into a safety position and checked his vitals. There was little sign of life but for his wild breathing: he was stiff as stone, his eyes were shut, his lips were blueing. I reached inside his jacket pockets and it all fit together — not just the current episode but the person he’d become. They were stuffed with three syringes, bloodied tissues, foundation cream, and silverware caked with Canada’s deadliest drug — a synthetic compound so potent that two milligrams (imagine two grains of salt) could murder a first-timer. Or a relapser.
Tyson had been clean for a couple months, but the stress of his new job was getting to him. Every Alberta number in his phone was exhausted for his go-to pills, but all he could find was heroin, unaware that it was laced with the new king of opioids.
It becomes easy to convince yourself that you’re untouchable.
The bad vibes started at the dealer’s door. She couldn’t answer simple questions about her product, which was white, not tan like the smack he’d done before. The vinegar-like “heroin smell” was too mild and he couldn’t reference any of her customers to be safe. Afraid to shoot up alone, Tyson schemed to use it at my house, unbeknownst to me. “I had one more bad vibe before I injected it,” he recalls, “but the further you go the harder it is to stop.”
The last thing he remembers is trying to hold himself up and call someone. “Thirty seconds later, I realized I was exactly where I knew I could end up.” That is, surrounded by eight paramedics, intubated, shirtless and shot in the shoulder with an opioid blocker that stopped the poison in its tracks.
Tyson was fucking lucky. By that November evening, fentanyl was killing almost a person a day in Alberta, more than in any other province, and ravaging thousands more families across North America who got tangled into it by a pharmaceutical system run amok. It’s an epidemic 20 years in the making.
*Not his real name. Other personal details have been changed to protect his identity.
•••
THE FIRST TIME MARLISS TAYLOR heard of fentanyl was 2006, after reading about an outbreak of fentanyl-laced heroin overdoses in New York. As a nurse by trade and the program manager of Street Works, Edmonton’s needle exchange on the downtrodden edge of downtown, she has one foot in healthcare and one in skid row. And in both worlds in Alberta, the preferred opioids were oxys and hydromorphones — popped, snorted, injected — but rarely heroin. So she filed away the memory and continued her harm-reduction work: dispensing syringes, portable sharps containers, and, just in case, vials of naloxone, the anti-opioid better known as Narcan.
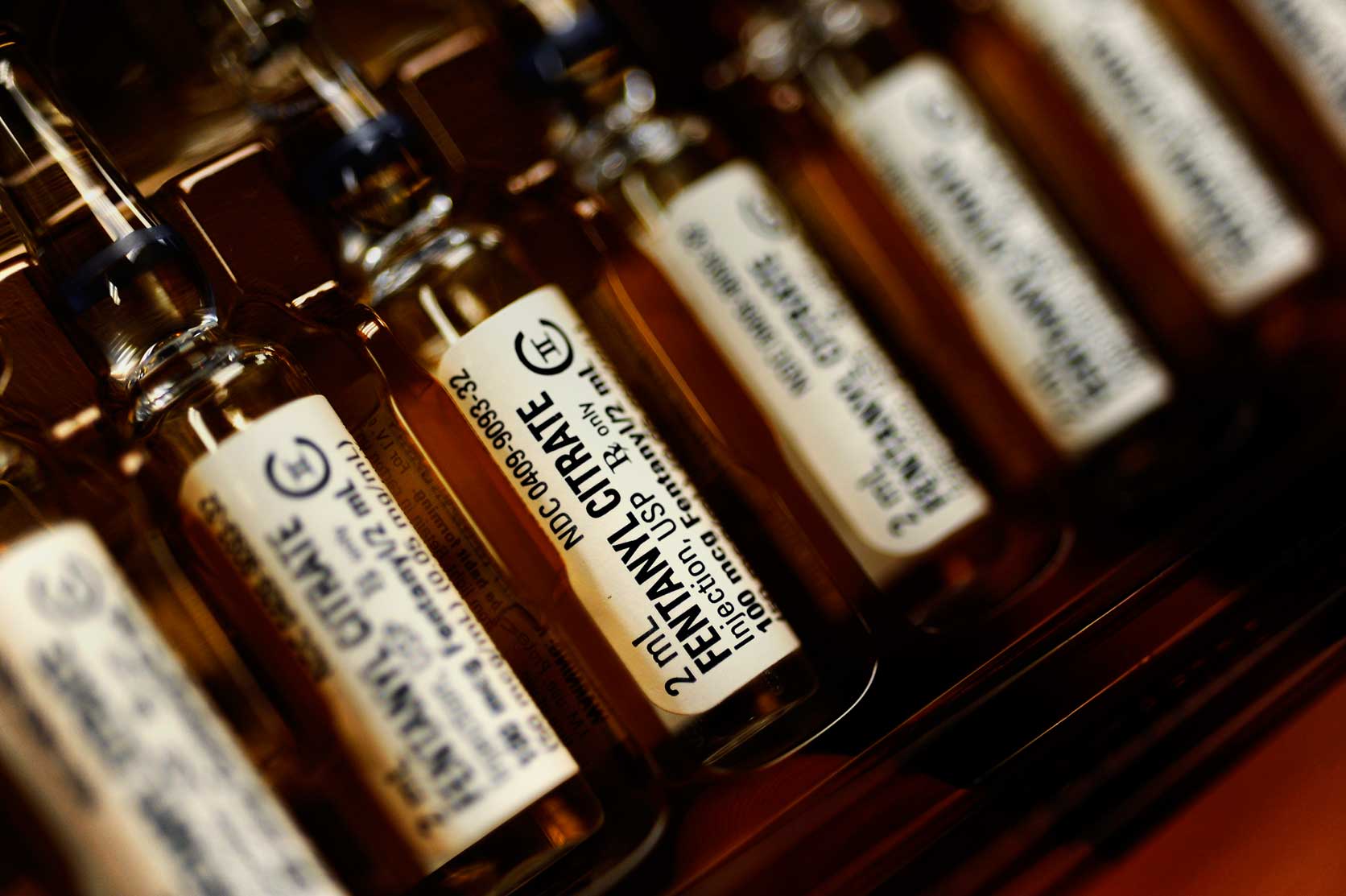
That was also around the time that Purdue Pharma, the maker of OxyContin, was in deep trouble with the US Federal Drug Administration bureau. The corporation sold its flagship product, launched in the mid ’90s, to doctors and patients as a safe painkiller, despite the semi-synthetic ingredient, oxycodone, being molecularly akin to heroin. Other “oxy” brands fol- lowed, and their manufacturers, like Purdue, downplayed the addictiveness. In 2007 Purdue pled guilty to marketing deceit and was fined $600 million — about half of what it made off the drug in a single year. By 2012, the year Canadian provinces started delisting OxyContin from healthcare coverage, 18.3 million opioid prescriptions had been filled in Canada, according to Pain Physician Journal. Those who weren’t satisfied with tamper-proof replacements, like OxyNeo (it’s uncrushable and turns goopy when liquefied, so it’s harder to abuse), or who had been cut off by doctors, or who’d always bought their oxys illegally, started turning to its synthetic cousin, fentanyl — the world’s most powerful painkiller.
Fentanyl’s been around since the ’60s as an anesthetic and pain reliever. There are fentanyl patches, sprays and lozenges. Mouth cancer patients suck on raspberry fentanyl lollipops. Because of its high potency — it’s 100 times stronger than morphine and 30 times stronger than heroin — it’s usually a doctor’s last resort. But despite its strength, it’s completely synthetic and, thus, remarkably cheap to produce. So as North American restrictions on oxycodone tightened, illicit fentanyl labs in Mexico and Asia happily picked up the slack with pure powder or green pills posing as oxys.
“Within a week around this building, violence went up,” says Taylor, recalling April 1, 2012, the date OxyContin was effectively banned. “Within two weeks, heroin and fentanyl were pouring into the city because [governments] were doing nothing to deal with the reasons people were using. They simply removed something people needed on a daily basis, so no surprise a market opened underground. Then we started seeing the sweep of fentanyl deaths.”
Killing your clientele seems like a terrible business plan.
Canada’s known fentanyl-implicated death toll between 2009 and 2014 was 1,019, according to the Canadian Centre on Substance Abuse and medical examiner offices. Over six years, Ontario’s body count nearly doubled to 149, making it the number one opioid killer. BC’s quadrupled to 49 in the year following OxyContin’s delisting, and it’s now traced in one third of the province’s fatal overdoses. And then there’s Alberta.
Isolated from US and port trafficking, dealers in the province were slow to get their hands on fentanyl, which is often smuggled from Mexico in heroin or shipped pure from China. But its availability was inevitable and when it arrived the carnage was exponential, from six deaths in 2011, to 66 in 2013, and 272 last year. “It started off as a trickle and the tap just kept opening more and more,” says Edmonton police detective Guy Pilon, who’s been on the drug and gang unit since 2002. “It’s killing more people than any drug that I’ve seen.”
The crises in the heartland has been cooked up from a mix of overprescribing, failed drug and health policies and unscrupulous dealers stretching their supplies — and profit margins.
•••
THE FIRST TIME DET. PILON seized fentanyl was three years ago, though he didn’t know it at the time. The word just showed up on a certificate of analysis, a report for every seized drug’s ingredients that’s produced for the courts. At the time, the opioids of the streets were illicit Oxy-80s, an OxyContin knockoff known as “fake oxy,” “shady 80s,” “green beans,” and many more monikers. “We were sending Oxy-80s and it was coming back as oxycodone,” says Det. Pilon. “But then, one day, it starts to come back as fentanyl.”
By now anyone buying oxys illegally in Alberta ought to know that they’re buying fentanyl because the real stuff’s been supplanted. (“Only an amateur wouldn’t know the difference,” says Tyson.) But fentanyl is also showing up in other drugs, like cocaine and ecstasy, and especially heroin. “I’ve never seen something that’s been in so many drugs,” says Pilon. Edmonton police are so concerned about accidentally inhaling or absorbing the transdermal drug that they wear hazmat suits during confiscations and carry Narcan for themselves.
But no city’s police officers have been kept busier by fentanyl than Calgary’s. It killed at least 81 Calgarians last year and, according to local police, about two-thirds of overdose scenes were in the suburbs. “It’s not just a phenomenon happening to entrenched drug users downtown,” says Dr. Nicholas Etches, the city’s chief medical officer of health. “It’s a phenomenon happening behind many closed doors throughout the province.”
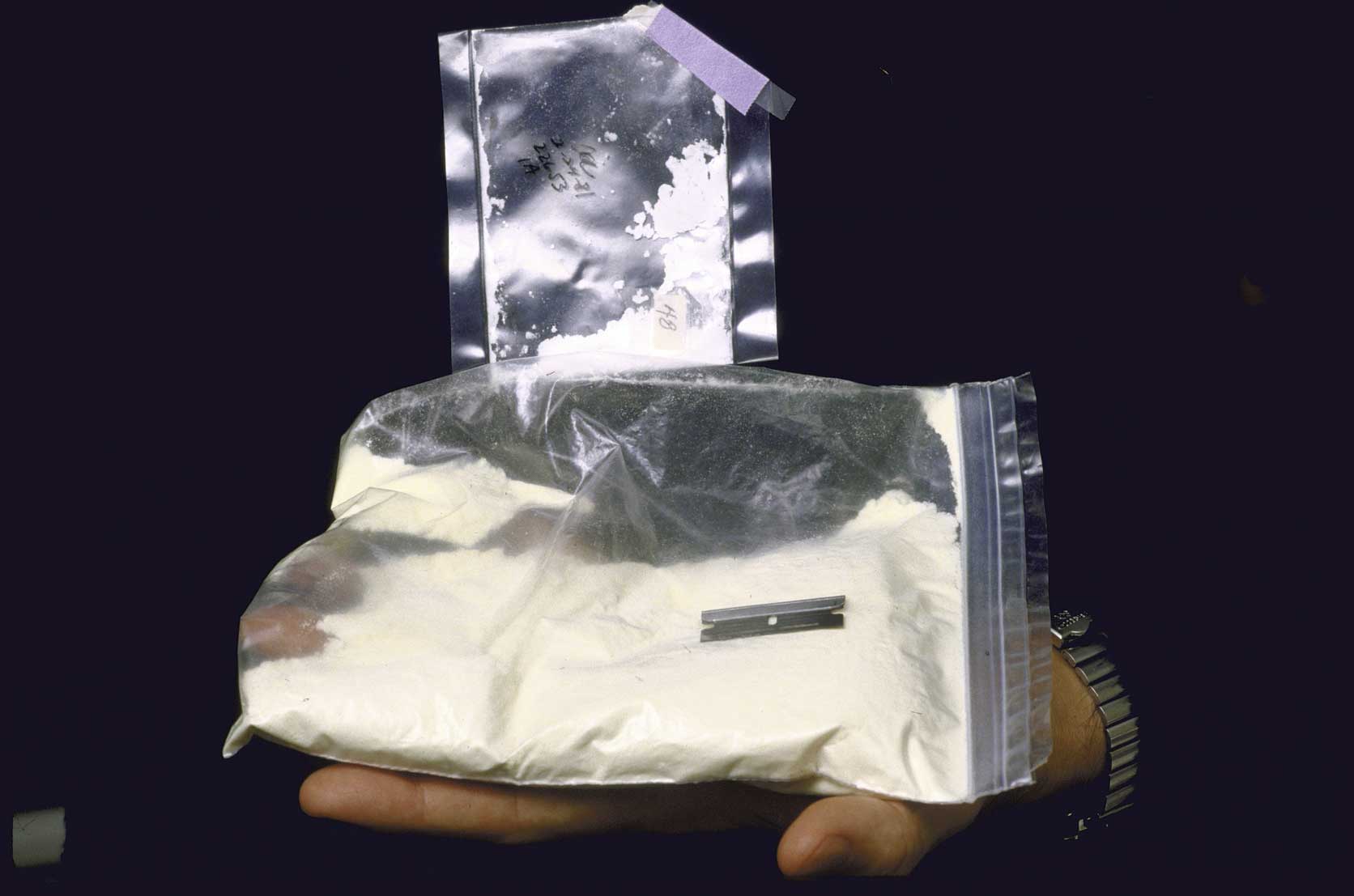
In the United States, where the rate of fatal fentanyl overdoses is much higher, the focal point of the crisis is blue-collar regions with frequent workplace injuries, like New Hampshire. This may also be true of Wild Rose Country. The province already has a proclivity for opioid prescriptions. A 2011 study by Canadian Family Physician found that Albertan doctors and pharmacists consistently dispensed more high-dosage opioids — 1,133 units per 1,000 people — than their Canadian counterparts in every province but Ontario. (Ironically, Alberta’s fentanyl dispensing was then the lowest in Canada.) But addicts unable to procure prescription drugs for whatever reason will have a harder time finding a proportionate substitute in Alberta. Although Tyson was able to score heroin, it isn’t as widely available here as it is in Toronto, Montreal or Vancouver, so many looking for an oxy replacement graduate straight to fentanyl, putting them at great risk of overdosing. “Honestly, if I could, I would get OxyContins back,” says Marliss Taylor of Street Works, which now dispenses double the amount of needles it did five years ago.
When it arrived the carnage was exponential, from six deaths in 2011, to 66 in 2013, and 272 last year.
Another factor is the West’s fentanyl stock itself. Eastern Canada is flush with pharmaceuticals like patches, diverted from prescriptions or pharmacy robberies. “Therefore, those individuals can predict the dosage,” explains Dr. Matthew Young, senior research and policy analyst for the CCSA. But he says out West it’s mostly powder, either cut with heroin or sold in capsules, meaning the potencies aren’t just high but wildly inconsistent. The dosage of two equal sized pills could vary by 3,500 micrograms, but since it’s so cheap and easy for illegal labs to manufacture, the difference means little to them.
What puzzles police, medical professionals and policy-makers alike is why street-level dope dealers would sell such an unforgiving drug in the first place. Killing your clientele seems like a terrible business plan.
But, like users, dealers have little say in their opioid supply. Unlike weed, it’s rarely, if ever, made in Canada. Much of the country’s heroin is in fact traced to the world’s biggest drug operation — El Chapo’s Sinaloa — which has embraced fentanyl to keep its “China White” competitive. Asian knockoff pills are deceptively professional. Likewise, locally filled capsules give false impressions of quality control. “Let’s say you have powdered fentanyl and you want to make each pill have an equal dose,” explains Dr. Young, “that’s a pretty complex chemical operation. They’re probably trying to make an equivalent dosage, but the adequate time and expertise isn’t there.”
There’s another way to look at it: imagine you’re a longtime user. Your tolerance is the highest its ever been. You’ve probably survived a few of your friends and maybe an overdose of your own. It becomes easy to convince yourself that you’re untouchable. “When most people are going through a destructive addiction,” Tyson tries explaining to me, “they tend to have an invincible feeling, like they know what they’re doing. I thought I was being smart with it.”
•••
AS FAR AS TYSON KNOWS, that night he nearly died on my floor was his first time with fentanyl, but it was not his first overdose, and, much more importantly, it was not his first relapse. Over the years he’s cycled through using, abusing, getting sober, then getting fucked up again. He says he’s been clean since November, but he also knows the odds are against him. “Realistically, I can relapse at any time,” he tells me in a phone call just days after his 30th birthday. “Am I going to? I’m 99.9 per cent sure that I won’t, but you have to hold that 0.1 per cent.”
It’s the most honest and lucid Tyson has been in years. Though how much can I really trust someone who’s barred from my house? It was easy to forgive his lies when they were contained on the other side of the country, but I’m still not over his utter disrespect for our home and lives. That entire visit — the happy greetings and hugs — all a pretence to shoot up and leave me and my wife with the consequences. Then I remind myself: it’s also the only reason he’s alive today.
Tyson is trying to rebuild trust with loved ones and mend what remaining positive relationships he has. He sees a psychiatrist, who diagnosed him with ADHD and is treating his anxiety. But he’s stopped short of entering rehab and doesn’t think he can be trusted on methadone. So I worry. Cold turkey treatments have only worsened Canada’s crisis, because relapsing on any high-dose opioid, but especially fentanyl, can be instantly lethal after a period of abstinence. It’s how Tyson landed on my floor in the first place. “That’s why the best treatment, by a long shot, is replacement therapy with either methadone or suboxone,” Dr. Michael Trew, who leads Alberta’s addictions and mental health services, tells me.
Because abstinence-only treatments have failed so many Albertans, the government’s reevaluating access to methadone and suboxone — essentially the most regulated pharmaceutical drugs, with only 35 doctors province-wide qualified to prescribe them and a wait time of up to eight weeks. The province has also followed Street Works’s lead by expanding Narcan availability. The Edmonton needle exchange centre was once the only social agency in Alberta to carry it, but as of January these life saving kits are being dispensed at social service agencies and prescribed to heavy users. In that sense, the street-entrenched might be further from fatally overdosing than people like Tyson, who does not carry naloxone, who didn’t even know how to get it.
Instead he’s trying to focus on life’s positive influences — family, friends, art, work — that, so far, have outsized his urges. “There was one time where I thought about it for 10 minutes, should I get a pill?” Tyson was gripping his phone tightly in his lap. He knew exactly who to call. He unlocked the screen and found the contact.
“Then I just deleted the number,” he says. “It felt really good.”



